All You Need To Know About Osteoporosis And How To Keep Your Bones Strong
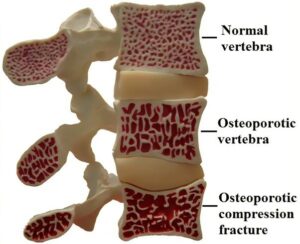
Osteoporosis is a condition where bones lose important minerals such as calcium quicker than they can be replaced by the body, resulting in a decrease in the thickness or density of bones. This can lead to them becoming fragile & brittle, and at a higher risk of fractures than normal bone. Often called the “silent disease”, osteoporosis can occur without any signs or symptoms until a bone fracture or break can be caused by even a minor bump or accident. Over time, these fractures can lead to changes in posture (eg. developing a stoop in your back), loss of height & muscle weakness.
HOW IS OSTEOPOROSIS DIAGNOSED?
Osteoporosis is diagnosed by measuring the mineral density of your bones (usually at the hip & spine) through a dual energy x-ray absorptiometry (DXA) scan, & this will enable doctors to determine the extent of bone loss & if any action is needed to improve your bone health. Finding out your bone density as early as possible is important so that you can take action to keep your bones strong, slow bone loss & decrease the risk of breaks. It is recommended that anyone over the age of 50 with risk factors should have a bone density scan, however some risk factors may also require people under 50 to have one.
WHAT ARE THE RISK FACTORS?
Risk factors for developing osteoporosis include: a family history, medical history, genetics, gender (females are at a higher risk), age of over 60 years, hormones, certain medications, smoking, low levels of exercise, high alcohol intake, being underweight, low calcium, low Vitamin D levels, certain types of cancer & some cancer treatments. For example, some breast cancer treatments reduce oestrogen levels which decreases bone density. The reduction in oestrogen level found during & after menopause is also why women are more likely than men to be diagnosed with osteoporosis & osteopenia.
WHAT ELSE CAN I DO TO KEEP MY BONES STRONG?
Certain types of activities are highly recommended to help improve & maintain bone density, including weight bearing activities & strength training. Weight bearing activities are ‘anti-gravity’ (against the resistance of gravity) exercises on land, & include jogging, running, jumping, hopping, skipping, stair climbing, dancing & any land-based sport.
Strength training includes any form of resistance or weighted training, as well as functional exercises that lift your own body weight. This type of activity provides the stimulus of both ‘compression’ on the bone from gravity & ‘traction’ on the bone from the attached muscles to promote stronger & healthier bones. Examples of such exercises include weighted squats & push ups.
HOW CAN CLINICAL PILATES HELP OSTEOPOROSIS?
Pilates is a form of resistance based exercise, particularly when done with specialised equipment. Exercises such as jumping using the Reformer jumpboard can provide a safe & controlled method of introducing impact to the bones without loading the joints as much as when performing the same activities on land. The improvement in muscle strength that comes with Clinical Pilates can also help to reduce the risk of falls & sustaining a fracture. This is further enhanced with the improvement of balance, coordination & reaction speed that can come with certain Pilates exercises.
Our physiotherapists at Inner Strength can develop an appropriate exercise program for anyone with osteoporosis, osteopenia or at risk of developing either, so contact us today!
Click here to book an appointment with a Physiotherapist.
Written by Jen Smith, Physiotherapist.